Key points
Symptom appearance
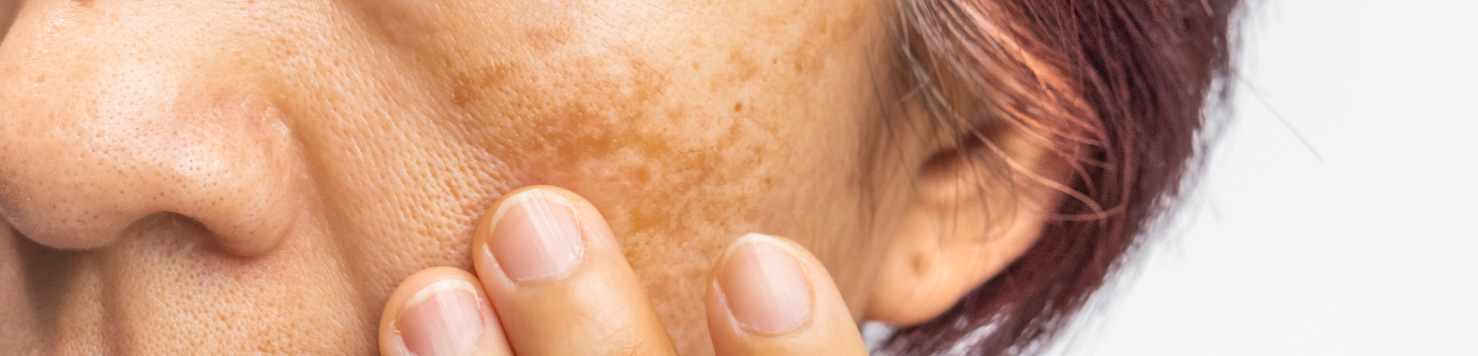
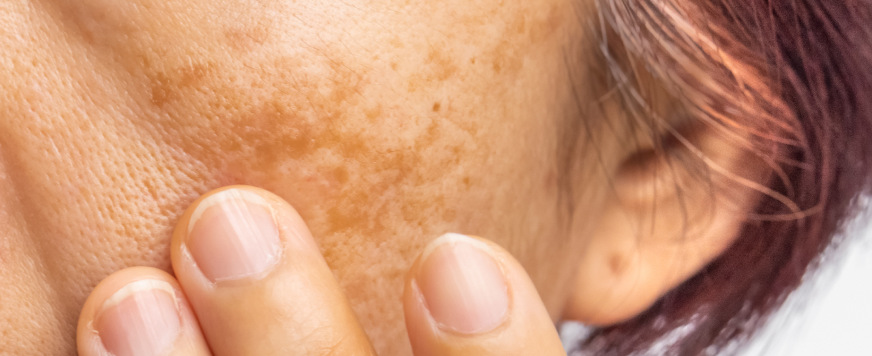
Melasma presents as brown, gray-brown, or tan patches on the face, most commonly on the cheeks, forehead, nose, and upper lip. Typically, the patches have a symmetrical distribution and may vary in size and shape.
Triggers
Sun exposure is a significant trigger for melasma. Specifically, UV radiation can stimulate the production of melanin (the pigment responsible for skin color), leading to the darkening of melasma patches. Moreover, hormonal changes, such as those occurring during pregnancy or with hormonal medications, can also contribute to its onset or worsening.
Diagnosis
A dermatologist can typically diagnose melasma based on a visual examination of the skin. Additionally, in some cases, a Wood’s lamp examination may be used to assess the depth and extent of pigmentation.